Frozen shoulder
Background
The condition is characterised by severe pain and loss of movement in the shoulder. It can be either primary (known as idiopathic) where the onset of symptoms is spontaneous. Secondary occurs when the condition follows a specific traumatic event, such as a tendon injury or after fracture. There is a spectrum of severity.
Frozen shoulder is more common in women than men and tends to occur between the ages 40 and 60. Frozen shoulder is more common in patients with diabetes, in total affecting 10-20% of people with diabetes.
The natural history of the condition is for the symptoms to resolve over time, this can be up to 3 years. However some reports state that improvement only occurs in 65% of patients
Key Features
- Severe pain
- Loss of active and passive movement
- ‘jerk pain’
- More common in diabetes
Symptoms
It is characterised by three phases. The length of each phase is variable.
- Painful phase
- Freezing phase
- Thawing phase
It begins with gradual onset of pain (painful phase) which can be severe, especially at night time. Patients usually complain of ‘jerk’ pain where sudden or unexpected movements produce severe exacerbations of pain. This can last several weeks to months.
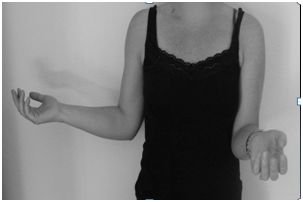
Next the shoulder becomes stiff (freezing phase), this stiffness occurs in all directions of movement but the hallmark is a reduction in external rotation as shown in the picture below. The pain can reduce at this stage but this is not always the case. The duration can be over 12 months.
Finally the movement of the shoulder improves (thawing phase), this often slow and gradual. There is debate about whether all patients return to normal function.
Clinical Assessment
The hallmark of the condition is pain and stiffness with restriction of both active and passive movements of the shoulder. This alongside a normal x-ray is how we make the diagnosis. MRI or ultrasound scan are usually normal unless there is suspicion of a rotator cuff tear as the underlying cause.
Picture shows loss of external rotation on the left.
Cause of stiffness
The shoulder is stiff because the shoulder capsule (lining) forms a contracture. This limits the available space for the shoulder to move in.
Treatment
All treatments must be compared to the natural history of the condition. In the painful phase physiotherapy may aggravate the situation. There maybe some inflammatory component in this stage, so an early steroid injection into the shoulder (glenohumeral) joint can be beneficial. However it may not effect the overall recovery.
Until pain begins to resolve exercises of the shoulder are best kept to within comfortable range of motion of the shoulder (see pendular and active assist exercise sheets). If pain is beginning to resolve then more aggressive stretching can be performed.
First Line treatments
The most common first line treatments used are a simple steroid injection into the glenohumeral joint followed by more more physiotherapy.
Distension Arthrogram is probably the most common intervention used at the minute where the radiologist injects contrast into the shoulder followed by a steroid injection and the injection of salt water fluid to stretch or cause a rent in the capsule of the shoulder.
Surgery
Surgery in the form of arthroscopic capsular release is usually a second line treatment.
Arthroscopic (keyhole surgery) release is a technique to surgically release the contracted tissue. This allows more precision than manipulation and results in less postoperative pain. Afterwards intensive physiotherapy is required to maintain the increased movement that is gained at surgery.
Generally by the end of the procedure movement can be restored, pain relief however may take up to 3 months to occur. Read more about surgery.
A Brooksbank

CONSULTING HOURS
CONTACT DETAILS
CONDITIONS
Treatment journey
APPOINTMENTS
Make a consultantion appointment wiith Mr Andrew Brooksbank at BMI Ross Hall Glasgow.
FAQ’s
Frequently asked questions about appointments, treatment, recovery and insurance/payments.

